EXI: Exercise Intelligence
Exercise. It’s a powerful thing. It can improve our physical and psychological health. It can manage, treat, and even prevent certain conditions. For many, it’s a life-changer.
For years, research has shown the benefits of physical activity, but we’ve never had the tools to release its full potential. Most healthcare professionals have been able to give recommendations, but not personalised prescriptions. Provide advice, but not incentivise or monitor real-time adherence. There has never been a seamless way to use exercise as a targeted and engaging treatment for all.
Until now.
More people.
More active.
More impact.
Engagement
At the core of everything we do is engaging people who are the hardest to reach, have low confidence in their ability to succeed and are quick to quit.
With multiple behaviour change methodologies embedded in the experience, e tap into personal motivations and empower sustainable lifestyle changes.
Personalisation
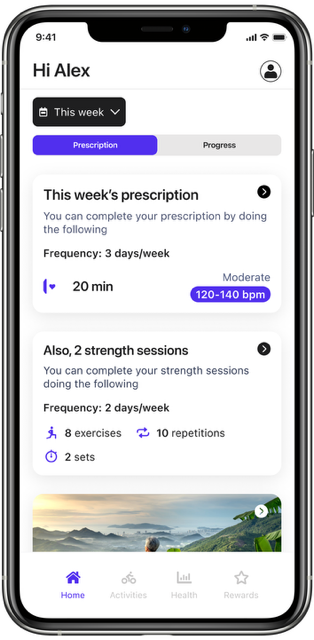
EXI is the only software to enable every person to automatically get a physical activity program that safely builds on the medical guidelines for multiple chronic conditions, medications, symptoms and activity levels.
We meet people where they are and the personal prescription adapts weekly to each person and their changing health status.
Health Outcomes
We use wearable technology to seamlessly track and trend the health improvements and costs savings for each member.
We track and trend the health improvements of exercise minutes, steps intensity, heart rate, weight, blood pressure, pain, fatigue, mood, symptoms and more.

Founded on
Science and Research
EXI is committed to scientific research that advances the credibility of digitally-delivered physical activity and behaviour change.
We partner with clinical and academic institutions to demonstrate the effectiveness of EXI in managing long-term health conditions and co-morbidities, both in terms of outcomes and adherence.
We prove that digital programmes are effective – when designed to reach every person, inspire engagement and improve population health.
We prove with industry research alongside our research that user characteristics and behaviours are associated with greater success on the EXI programme.
Led by Health Experts
A team with decades of experience in healthcare, physical activity and behaviour change.
A team with a vision of the world where the prevalence, cost and impact of long-term conditions is dramatically reduced thanks to physical activity as lifestyle medicine.








EXI is the Global MedTech Parther for the ACSM Exercise is Medicine® programme
“This best-in-class, intelligent platform has the capability of truly making an impact on the health care and fitness industries.”
ACSM CEO Kristin Belleson.
Learn More